According to scientists and certain optimistic enthusiasts, we might be ready to send the first…
Clinicards – The End of Medical Apps
There are times when a company reaches a tipping-point that determines its future course. Ford’s legendary T-model, Apple’s iPhone….when we poured our vision of mobile health into our first medical app (the ‘iP Plaslijst’ for urinary disorders) in 2012 we were only halfway there, but now, 4 years and 25 medical apps later we have almost reached that tipping-point.
With the soft launch of Clinicards, we are already lifting part of the veil. Medical apps can significantly help to improve health. It is a fact that 99% of the data generated by a person is generated outside of the clinical setting, mainly at home. This highly relevant data is usually unattainable for the patient as well as for the healthcare professionals. The current explosion of available health-related apps in the App Store/Google Play Store (close to 150,000) stand testament to the relevance of this data. This superabundance is in itself a problem, leading to choice anxiety and information fragmentation. Every app stores its data in a different vault and we need to think about how all that information can be combined.
After 4 years of app development, we realized that the majority of medical apps need to ask the patient ‘something’. That ‘something’ can be a pain-level rating, or in the case of our iP Plaslijst the number of urinations, volume, leaks and fluid intake. However, in the case of our ‘ReumaCoach’ (for rheumatism) we need to find out from the patient how active they have been (determined through a wearable), how much pain they experienced and which medicines they took. But what happens if a patient wants to know how many fluids they ingested as well as what their activity-levels are? Should they use 2 apps simultaneously? The answer comes in the shape of Clinicards!
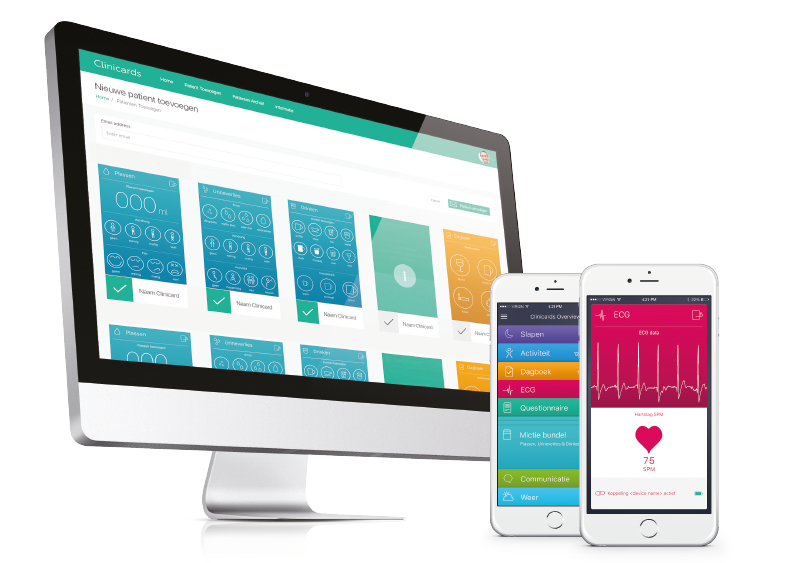
A Clinicard is 1 single functionality represented by a digital ‘map’ that only measures 1 clinical parameter. In the above mentioned case we would need 6 separate Clinicards: urinating, drinking and urinary leakage (the iP Plaslijst collection); pain, activity and medication (the ReumaCoach collection). What makes this setup unique is that the Clinicards can be indefinitely combined to perfectly suit the patient’s clinical portrait. The range will of course not be limited to these 6 Clinicards; it is our intention to develop a whole library of Clinicards. Every Clinicard falls into one of the following categories: Passive Data Collection (linked to a sensor/wearable), Active Data Collection (active input of data), Questionnaire, Communication (via chat and/or video calls), and External Data Source (for example a pollen database).
The patient can select the appropriate Clinicards together with his/her healthcare provider from a web portal. This provides the patient with the immediate opportunity to question why this or that is being measured, which in turn is a great stimulus for improving communication. The patient can download the selected Clinicards from the App Store, after which they will automatically appear in the app. Depending on their selection, the collected data can be recorded and the results will be comprehensibly displayed on the web portal, thereby enabling the patient to easily discuss the gained insight with his/her healthcare provider. The overarching principle is that the data is always the patient’s own data; it is always the patient who gets to decide what happens with the data and who has access to it. That can happen at a very granular level: Clinicard A for person X and Clinicard B for person Y. Naturally, the patients themselves can access their own data at any time in order to analyze their health status/evolution.
Using Clinicards is so simple that one can easily be fooled into thinking that their development is equally simple. Nothing is further from the truth! A Clinicard is a highly advanced piece of software and needs to comply with a plethora of requirements. A Clinicard must be: developed in collaboration with the corresponding specialized healthcare professionals, CE-certified, based on the latest standards of interoperability (health information building blocks or Detailed Clinical Model), and, if possible, linked to sensors and/or wearables. Nevertheless, it is more complex than building an app from scratch; the ICT architecture is already in place and so we can immediately jump into the more clinical aspects of the application. We are currently implementing a first application for the Slingeland Hospital, for which we have developed Clinicards to be used in the Cardiology Department for atrial fibrillation; the first private beta-version is ready for testing.
Please contact Erik van der Zijden (erik@synappz.nl or +31 6-109 30140) should you wish to obtain more information.




